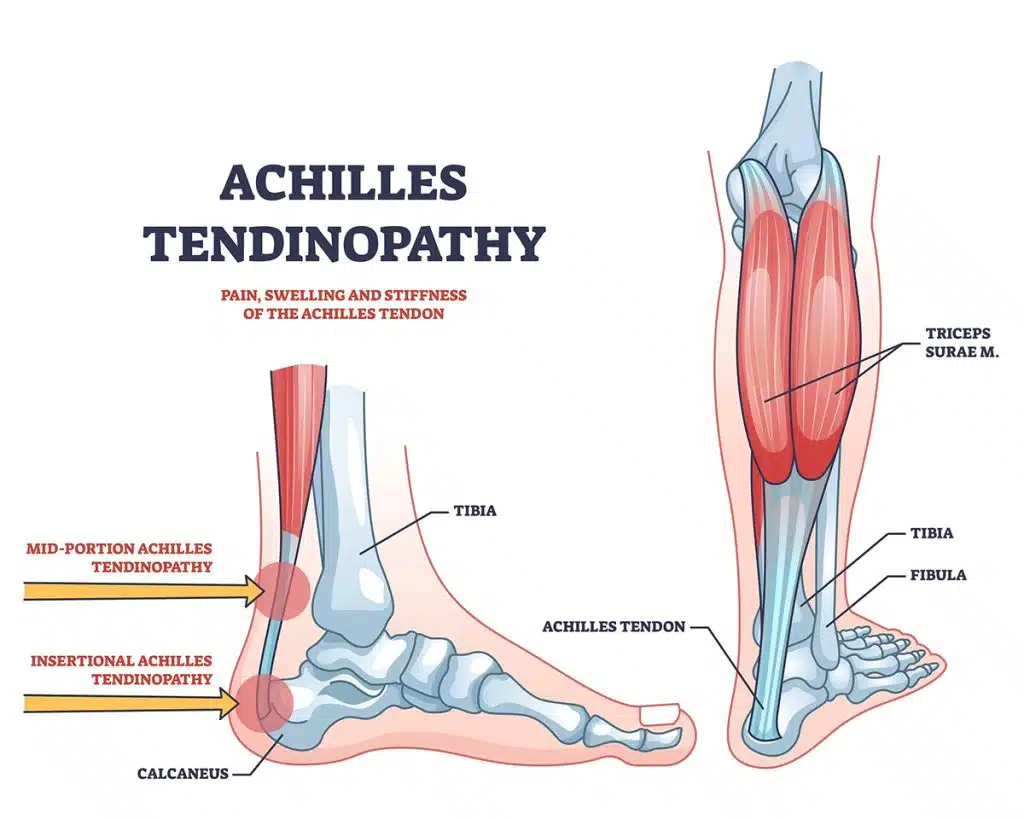
Why calf flexibility and eccentric loading matter
AAOS specifically highlights calf stretching and eccentric strengthening as important parts of treatment. Tight calves can place extra stress on the Achilles tendon, especially near the heel insertion. Eccentric strengthening, which means the calf is working while lengthening, can help the tendon tolerate load better when used appropriately.
This is a big reason self-treatment often falls short. People rest until the pain is less intense, then return to the same pattern without rebuilding flexibility or tendon capacity. The result is a cycle of partial improvement followed by another setback.
A structured plan can help restore ankle motion, reduce morning stiffness, improve calf strength, and guide a safer return to walking, gym activity, court sports, or running. The point is not just pain reduction. The point is making the tendon more dependable again.
What to know about injections and other options
Patients often ask whether an injection can make the problem go away faster. AAOS warns that cortisone injections into the Achilles tendon are not recommended because they can weaken the tendon and increase rupture risk. That is an important distinction. A treatment that helps in other body areas may be a bad idea in this tendon.
AAOS also notes that other injectable treatments, such as platelet-rich plasma, have been studied, but the evidence is still evolving. In some cases, extracorporeal shockwave therapy may also be discussed. Recent studies have shown potential improvement in pain and function, particularly when paired with other nonsurgical strategies, though AAOS notes that more information is still needed before strong routine recommendations can be made.
The right takeaway is not that every newer option should be pursued. It is that these decisions should be made in the context of the actual tendon problem, not marketing hype or desperation after a few bad weeks.