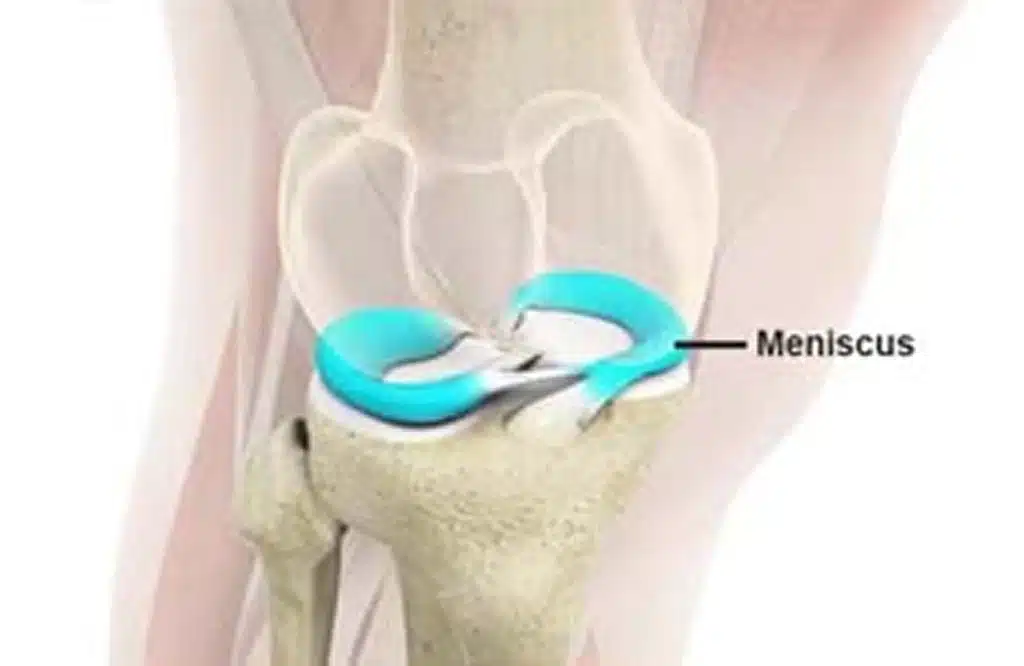
Why meniscus symptoms can overlap with other knee problems
Another reason evaluation matters is that several knee conditions can sound similar at first. Arthritis flares, ligament injuries, patellofemoral pain, loose bodies, tendon irritation, and cartilage injury can all create overlapping complaints. A person may describe pain, swelling, or a catching sensation, but the actual pain generator may not be obvious without an exam.
That is especially true when arthritis and a meniscus tear show up together. Imaging might reveal both, but treatment still has to focus on the real symptom driver. Sometimes the tear is the main issue. Sometimes the broader knee environment matters more.
This is where a patient-first orthopedic approach helps. Instead of chasing one scan term in isolation, the goal is to make sense of the whole knee and match treatment to how the symptoms behave in daily life.
How to think about the next step if your knee is not improving
If the knee is staying swollen, repeatedly catching, limiting work or activity, or making normal walking feel unreliable, it is worth getting assessed. The longer a person spends bouncing between rest, internet advice, random braces, and short-lived improvements, the easier it is to lose momentum and confidence.
The next step does not have to mean surgery. It can simply mean getting clarity. Once you know whether the pattern fits a meniscus tear, whether imaging is needed, and whether the knee looks more like a rehab case or a surgical discussion case, the path forward usually feels much less overwhelming.