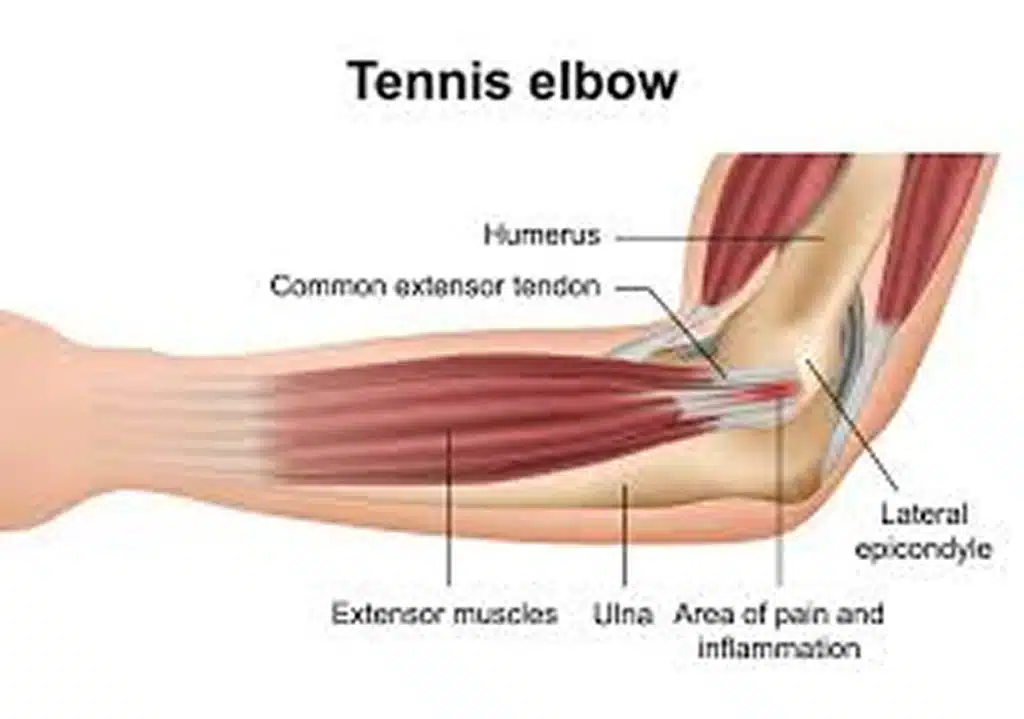
Why therapy and exercise matter more than many people expect
AAOS points out that physical or occupational therapy can be especially helpful, including specific exercises to strengthen the forearm muscles. Therapists may also use modalities like ultrasound, ice massage, or muscle stimulation, but the bigger value is usually a structured plan for rebuilding movement capacity.
That matters because tennis elbow is often aggravated by how force is transferred through the wrist, forearm, and elbow. If the muscles fatigue too quickly, if technique is poor, or if the tendon is reloaded too aggressively after pain settles down, symptoms can linger.
A thoughtful rehabilitation plan can help patients rebuild gripping tolerance, adjust movement patterns, improve forearm endurance, and return more gradually to lifting, racquet sports, golf, typing-heavy work, or manual labor. For many patients, the difference between a long-running problem and a turning point is not one dramatic treatment. It is consistent load management done well.
What to know about braces, injections, and newer options
Forearm straps or braces can help in selected cases by reducing strain on the involved tendon. AAOS notes that a brace centered over the back of the forearm may relieve symptoms by giving the muscles and tendons more rest. This does not fix the whole problem on its own, but it can be useful as part of a larger plan.
AAOS also discusses steroid injections, platelet-rich plasma, and shock wave therapy. Steroid injections may reduce symptoms because they are powerful anti-inflammatory medications, but AAOS warns they should be used sparingly because excessive use may weaken the tendon attachment over time. That is an important tradeoff and one reason quick pain relief is not the only decision point.
Platelet-rich plasma has shown mixed but sometimes promising findings. Shock wave therapy is still considered experimental by many clinicians, though some sources suggest it may help. The key is that not every patient with tennis elbow needs every treatment option discussed online. The most useful next step depends on how long symptoms have been present, how the tendon is behaving, and what conservative care has already been tried.
When surgery becomes part of the conversation
Surgery is usually reserved for cases that do not respond after a meaningful course of nonsurgical care. AAOS says surgery may be considered if symptoms do not improve after 6 to 12 months of conservative treatment.
Most surgical procedures involve removing diseased tendon tissue and reattaching healthier tendon back to bone. AAOS describes both open and arthroscopic approaches, along with risks such as infection, nerve or blood vessel injury, prolonged rehabilitation, loss of strength, loss of flexibility, and the need for further surgery.
That does not mean surgery is a bad option when it is truly needed. It means the decision should be made carefully, with a realistic view of rehab and expected recovery. Most patients would rather avoid it if a strong nonsurgical plan can get them back to daily life and activity.